I am a Radiological Medical Practitioner
- Be satisfied that the necessary clinical information is not available from the patient’s previous examinations, or from any other alternate medical tests or investigations not involving the use of ionizing radiation.
- Be conscious of the patient dose and for any given examination shall attempt to be in line with international reference levels or those recommended by the regulatory body.
- Periodically evaluate medical procedures for possible reduction of doses, especially for paediatric procedures.
- Monitor patient doses in CT and Interventional Radiology procedures and provide radiation dose reports to the patient.
- Counsel the patient for probable effects of radiation in complex radiological procedures.
- Customize the exposure protocols to obtain optimum image quality with minimum patient doses
- Undergo equipment specific training through the supplier prior to commissioning of X-ray equipment, and specifically for Interventional Radiology and Computed Tomography equipment
- Undergo training provided by the RSO towards radiation protection and optimization of patient doses.
Radiation Protection in Pediatric Radiology
Introduction:
- Skull radiograph in an infant or child with epilepsy;
- skull radiograph in an infant or child with headaches;
- sinus radiograph in an infant or child under 6 years of age suspected of having sinusitis;
- cervical spine radiograph in an infant or child with torticollis without trauma;
- radiographs of the opposite side for comparison in limb injury;
- scaphoid radiographs in children under 6 years of age;
- nasal bone radiographs in children under 3 years of age;
- routine daily chest examination in intensive care units;
- Radiological examinations requested purely for medico-legal purposes
- By being wary of “unfavorable conditions”;
- Through proper choice of equipment;
- Through proper operational procedures for different modalities.
- Using unsuitable Automatic Exposure systems; in imported equipment, which are not customized to Indian demography before use;
- Following adult exposure protocols for children;
- Using sub-standard equipment, which has not been design approved (AERB Type Approved) and not subjecting the equipment to periodic quality control tests;
- Not using all dose-minimizing features that the machine provides;
- Radiographs taken by unqualified personnel, who do not fully appreciate the implication of their actions;
- Not considering alternate means of diagnosis (MRI, USG etc);
- Not asking for previous x-ray records, for same ailment; Expecting best quality images, even if there is no additional gain in terms of diagnosis; Unnecessary referrals.
- Do not buy refurbished equipment from un-authorized suppliers:
- Such equipments are not design approved by AERB.
- The equipment shall be AERB Type approved
- High frequency and high power (kW) equipment, i.e. higher mA (> 300 mA) stations should be preferred (facilitates to use shorter exposure times and reduced retakes)
- small focal spot of about 0.5 mm - 0.8 mm
- removable anti scatter grid
- AEC (Automatic Exposure Control) provision with proper calibration of paediatric protocols carbon fiber couch
- patient dose recording option is recommended for continual monitoring and optimization
Proper operation procedures:
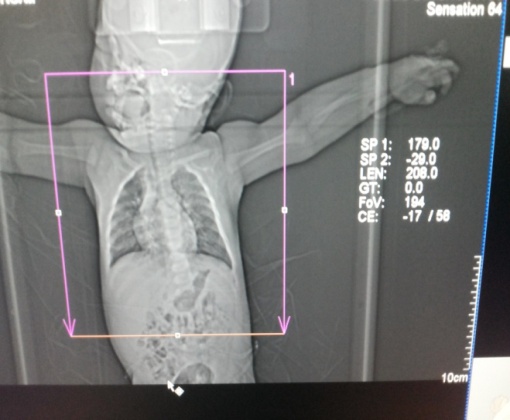
- AVOID “Babygrams”. Expose only areas of interest
- Replace faulty collimator bulb immediately. Not having a light beam as a guide could result in the complete opening of collimator an infant and cause whole body exposure. (see below a representation)
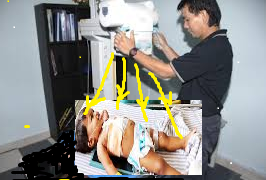
Optimization in Radiography
- Use shielding and immobilization devices: These devices help towards correct collimation, and proper positioning of shielding devices, to protect radiosensitive organs such as gonads, breast, eye lens and thyroid.
- Judiciously use Anti-scatter grid:Anti-scatter grid is used for reducing scatter radiation, thereby improving the image quality. The flipside of using these grids is the need for higher exposure parameters. For children doseis increased 3-5 times without any concomitant improvement in image quality.
-
Identify “child-friendly” parameters of exposure: High kV, shortest exposure time and high mA (for required mAs), more focal to film distance and use of additional filters are important.
Fluoroscopy and Interventional Radiology
IR procedures can cause deterministic injuries. Hence, paediatric interventional procedures may be performed by experienced paediatric interventionists and assisted by qualified and trained technologists in radiological protection.
Use “Child- suitable” IR equipment:- Conscious use of collimators is a must.
- Use lowest dose protocol possible for patient size, frame rate (3.5–7.5 pulses/s for pulsed fluoroscopy) and length of run (in cine mode). Image acquisition runs should only be performed if necessary,
- “last image hold” option
- Tube to patient distance should be maximized and patient to detector should be minimized.
- Fields need to be tightly aligned to area of interest using light beam diaphragm
- Minimize electronic magnification; digital zoom needs to be used whenever possible.
- Position imageintensifierand/orreceptorpositionedovertheareaofinterestbefore fluoroscopy is commenced rather than during fluoroscopy.
- Fluoroscopy timing alerts
Computed Tomography
A high quality of image is not always necessary. Higher Image quality (at the cost of higher exposure parameters) is opted for, more out of habit, than as a requirement for confident diagnosis.Noise reduction means high doses; noise is acceptable if the scan is giving the diagnostic information.
Watch out for these pitfalls:
- Scan only the required lengths and minimize the scanning of identical areas.
- Do not give same exposure factors for pelvic (high contrast region) as for abdomen (low contrast region)
- Use spiral scan with a pitch greater than 1(e.g.1.5), provided this does not automatically increase the mA.
- Thicker collimation with overlapping reconstruction needs to be used when thin slices are not needed.
- Avoid major overlap when scanning adjacent areas with different protocol.
- Use reconstruction wherever possible, for different slice thicknesses.
- Single phase scans are often adequate. Pre- and post-contrast or delayed scans rarely give additional information in children but can double or triple the dose
- Avoid increasing volume covered in a particular examination (Z axis over-beaming) causing extra rotations and effect of penumbra.









